Wisdom teeth are the third molars at the very back of the mouth. They usually try to erupt in the late teens or early 20s because that’s when the jaw finishes growing. If you’ve been wondering how to tell if your wisdom teeth are coming in, this post walks through common signs, simple home care, when symptoms indicate a problem, and what treatment options look like. Expect clear signs to watch for, what to do at home, and when to see a dentist or oral surgeon.
How do you know your wisdom teeth are coming in: common early signs
Gum pain or tenderness behind the last molars
A common first sign is dull, aching pain or soreness at the back of your mouth. You may feel tenderness when touching the area or when chewing. This is often the gum reacting to a tooth pressing from below as it pushes through.
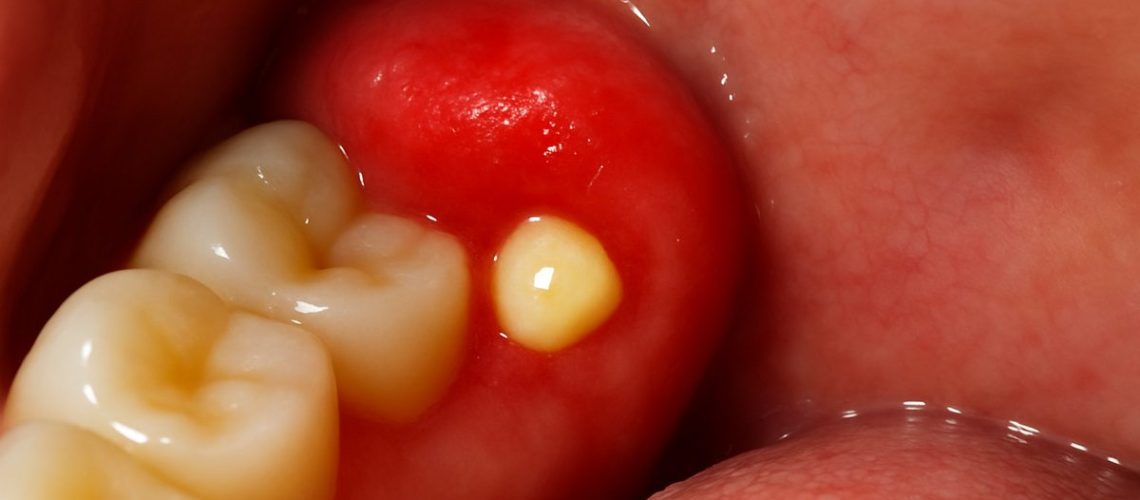
Redness, swelling, or a small bump on the gum
You might notice localized swelling or a raised flap of gum tissue (an operculum) over a partially erupted tooth. The tissue can be red and tender. This happens when the tooth breaks the surface unevenly, leaving an area where food and bacteria can collect.
Bad taste, bad breath, or pus drainage
If food gets trapped under a gum flap, bacteria can build up, leading to a bad taste or persistent bad breath. In some cases, you may see or taste a small amount of pus. These signs point to trapped debris and early infection under the gum.
Jaw stiffness, ear pain, or headaches
Pressure from erupting wisdom teeth can cause jaw ache or stiffness and may radiate into the ear or temples. This referred pain occurs because of shared nerves and tight jaw muscles reacting to the new tooth as it tries to find space.
Changes in bite or crowding
You may feel pressure against the second molars, notice sensitivity when biting, or sense slight shifting of nearby teeth. Wisdom teeth can push on adjacent teeth as they come in, producing pressure-related discomfort and, in some cases, minor crowding.
Signs that mean you may have an infection or a problem
Severe pain, fever, or swollen jaw/face
Intense pain with fever or noticeable facial swelling is a red flag for a more serious infection and needs prompt evaluation. These symptoms suggest the infection is significant and likely won’t resolve on its own.
Difficulty opening your mouth (trismus) or swallowing
If you can’t open your mouth fully or have trouble swallowing, call a provider right away. Limited mouth opening can signal the spread of infection into the jaw muscles or surrounding tissues and may require urgent treatment.
Visible pus or rapidly spreading swelling
Pus, increasing redness, or swelling that spreads quickly beyond the immediate area are urgent signs. Rapid progression risks deeper tissue infection and may need antibiotics plus a surgical visit to drain or remove the source.
How long symptoms last and what to expect
Typical timeline for eruption vs. persistent problems
Wisdom tooth soreness is often short-lived—days to a couple of weeks—as the tooth breaks through. If pain or swelling returns frequently or lasts longer than a few weeks, it suggests ongoing impaction, repeated infections, or damage to nearby teeth that likely needs treatment.
Why do some people never have symptoms?
Many people never notice their wisdom teeth. If teeth are well-positioned and fully erupted, or if they remain buried without causing pressure, they may remain asymptomatic and not require removal.
Home care while your wisdom teeth are coming in
Pain relief and swelling control
Over-the-counter ibuprofen or acetaminophen can reduce pain and inflammation—follow package dosing. Cold compresses applied to the cheek for 10–20 minutes at a time can help reduce swelling and discomfort. If you’re on other medicines, check with a provider before taking new pain relievers.
Oral hygiene and rinses
Rinse gently with warm salt water several times a day to help flush food and bacteria from around the erupting tooth. Brush gently near the back molars and avoid poking the gum flap with sharp tools or cotton swabs, as this can worsen irritation.
Diet and daily habits
Stick to soft foods if chewing hurts, and avoid crunchy, sticky, or tiny-seeded foods that can lodge near the erupting tooth. Don’t smoke—smoking delays healing and increases infection risk. Get rest and avoid strenuous activity while sore.
When antibiotics or a dentist visit may be needed
Antibiotics can temporarily treat a bacterial infection, but they don’t fix an impacted tooth or remove trapped debris. If infection recurs or if signs are severe, see a dentist or oral surgeon for a proper exam and imaging.
When to see an oral surgeon and what they will do
Red flags that require a surgical consult
See an oral surgeon for persistent pain, repeated infections, damage to nearby teeth, cysts on X-rays, or if the wisdom tooth affects orthodontic results. These issues often need surgical removal rather than simple fixes.
How surgeons evaluate wisdom teeth
An exam and dental X-rays, or a CBCT scan, show tooth position, root shape, and their relation to nerves and sinuses. This imaging helps the surgeon plan a safe, precise approach and explain risks and recovery expectations.
What removal options and sedation look like
Options range from simple extraction for fully erupted teeth to surgical removal for impacted roots. Sedation choices include local anesthesia, nitrous oxide, oral sedation, or IV sedation. Recovery usually involves a few days of rest, swelling control, and a soft-food diet.
About Texas Center for Oral Surgery & Dental Implants
Texas Center for Oral Surgery & Dental Implants serves the Dallas–Fort Worth Metroplex with board-certified oral and maxillofacial surgeons who offer 3D imaging, in-house sedation, and experience managing complex wisdom tooth cases. The team provides thoughtful, minimally invasive options and clear guidance from consultation through recovery.
Preparing for extraction and recovery tips
Before surgery
Bring ID, follow fasting instructions if sedated, and arrange a ride home. Share a full medical history and current medications so the team can plan safe anesthesia and pain control.
After surgery
Expect swelling and some discomfort for a few days. Use prescribed or OTC pain relief as directed, apply cold packs early, eat soft foods, and follow wound care and oral hygiene instructions. Contact your surgeon for signs of heavy bleeding, fever, or worsening pain.
Quick FAQ and closing guidance
Can wisdom teeth move back?
No — once a tooth erupts toward the mouth, it won’t “move back” under normal conditions.
When is removal urgent?
Persistent infection, spreading swelling, trouble breathing, or inability to swallow are urgent.
Are antibiotics enough?
Antibiotics can control infection in the short term, but won’t resolve an impacted tooth—definitive treatment is usually needed. If you’re unsure whether your wisdom teeth are coming in or you have concerning symptoms, schedule an evaluation with a board-certified oral surgeon for safe, expert care.